
Powered By





Many people with lupus develop rashes on their skin, including their legs. Lupus can affect different parts of the body, like the skin and organs. The most common type is systemic lupus erythematosus (SLE). Cutaneous lupus affects the skin and can happen by itself or along with SLE. Two types that can affect the legs are discoid lupus erythematosus (DLE) and subacute cutaneous lupus erythematosus (SCLE).
In this article, you’ll learn about the types of leg rashes that can happen with lupus, what causes them, and how to manage and treat them.
Skin rashes are common among MyLupusTeam members. Not everyone with lupus will have rashes on their legs. When they do happen, they can look different from person to person.
One MyLupusTeam member described their skin symptoms as “little things that look like blood blisters that then break open and start bleeding. When they heal, they leave scars and look horrible.”
Other lupus leg rashes may be described as faint, interlocking networks of red circles. For example, one MyLupusTeam member reported, “I get a rash with red lacy circles on my legs. It kind of looks like a snake pattern. It seems to show up when I’m having a flare and my hip joints and thighs hurt a lot.”
There’s as much variety in how lupus leg rashes feel as in their appearance. As one MyLupusTeam member observed, “There are so many different kinds of skin issues with this disease. We’re all so different but also alike.”
You may experience a painful burning, crawling, or pin-pricking sensation with a lupus leg rash. Some people describe it as feeling like a sunburn. Other MyLupusTeam members report increased sensitivity to either very hot or cold temperatures, which causes itchy or painful hives, chilblains (painful red or purple bumps from cold), blisters, or pimple-like bumps. Some people describe visible skin changes, while others have itching or pain without any rashes or changes in color.
Some lupus-related rashes are intensely itchy. Another MyLupusTeam member wrote, “By the end of the day, my skin feels like I have an army of ants under it, and I am scratching it till it bleeds.”
Lupus leg rashes can be hard to predict. Symptoms may come and go, and can change with the time of day, the season, or stress. Some rashes can last for months or longer if they aren’t treated.
It can take a toll on your emotions when skin symptoms affect your physical appearance and when other people have reactions to your skin issues. As one MyLupusTeam member wrote, “Because of the skin lesions, people stare at you… It not only takes a toll on your self-esteem, but it’s so painful as well.”
Living with lupus can be a stressful experience. Stress can make you feel overwhelmed and isolated. Seeking help from a therapist, counselor, or behavioral health provider can help you better cope with the social and emotional struggles of chronic skin problems.
Itching can disrupt sleep, increase mood problems, and lead to scratching and scarring. A MyLupusTeam member commented, “I also get lesions on my lower legs that are so itchy, my scratching breaks the skin or causes bruising.”
Lupus is an autoimmune disease, which means that symptoms happen when a person’s immune system attacks their tissues. This can include symptoms on the skin, like rashes.
The main triggers for rashes on the legs with lupus are:
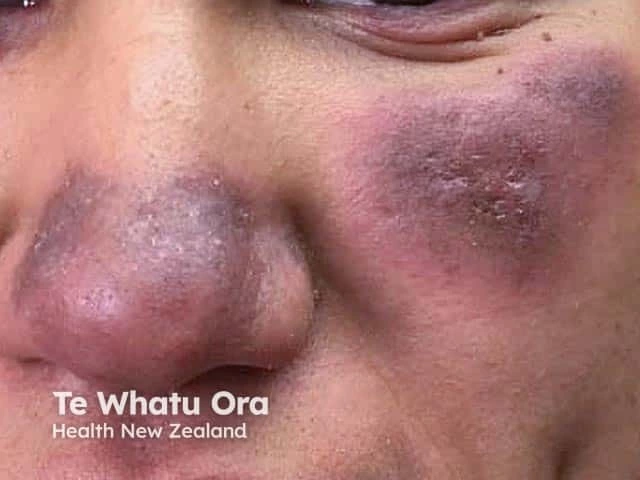
DLE can cause round, coin- or disk-shaped red patches that are thick and scaly. It may or may not itch or hurt and can lead to scarring, especially if scratched. Sunlight can also cause lasting discoloration (lighter or darker areas).
If you don’t already have a dermatologist, you can ask your primary healthcare provider for a referral. A dermatologist may perform a biopsy to confirm a DLE diagnosis. A biopsy involves removing a small sample of tissue or cells for examination under a microscope.
SCLE can cause circular red patches with a ring-like border that may be scaly. These rashes often show up on sun-exposed skin, including the legs, and usually don’t itch or cause pain.
Sunlight and taking certain medications can trigger SCLE. Doctors use the word “subacute” to describe this rash because it appears quickly and doesn’t last as long as other lupus rashes. SCLE doesn’t cause scarring like DLE, but can cause permanent skin lightening or darkening.
Because there are different kinds of lupus leg rashes, it’s important to see a dermatologist or other healthcare provider to help you get a diagnosis and find the right treatment plan for your rash. Before starting treatment, your healthcare provider may do a biopsy or other tests to find out what type of cutaneous lupus you have.
The main types of treatments for lupus rashes on the legs are:
MyLupusTeam members with skin symptoms recommend cool (not cold) baths, sometimes with oatmeal, to help soothe their itchy or painful rashes. Baths can also offer a relaxing way to prepare for a better night’s sleep if your leg rashes keep you awake.
While you can’t prevent cutaneous lupus, you may be able to prevent rashes with some lifestyle changes. Exposure to sunlight often triggers rashes and sores and makes breakouts worse. Avoiding sun exposure can be key.
Learning what triggers your rashes and how to avoid these triggers can help you experience less pain and itching from leg rashes.
Here are some tips for avoiding triggers and protecting your skin:
Lupus leg rashes can be frustrating, but there are steps that help. Keep track of flare triggers (like sun, cold, or stress) and talk with your care team about treatment options. If you have lupus and skin symptoms, see a dermatologist for regular skin checks. Also consider mental health support if your leg rashes lead to anxiety, depression, feeling isolated, or trouble sleeping. You don’t have to manage this alone. Support from your care team and community can make a real difference.
On MyLupusTeam, people share their experiences with lupus, get advice, and find support from others who understand.
How have you managed leg rashes with lupus? Let others know in the comments below.
Get updates directly to your inbox.



The Rash On My Legs Looks Just Like The One Pictured, But Has Lasted A Couple Of Years. Is This Normal. I Have Been Recently Diagnosed.
Become a member to get even more




This is a member-feature!
Sign up for free to view article comments.
A leg rash is my first warning of a flare. The progression: A red rash appears on one or both lower legs, always in the area between my knee and ankle. If the rash is on both legs at the same time, I… read more
We'd love to hear from you! Please share your name and email to post and read comments.
You'll also get the latest articles directly to your inbox.